Isoflurane Anesthetic Properties and Uses
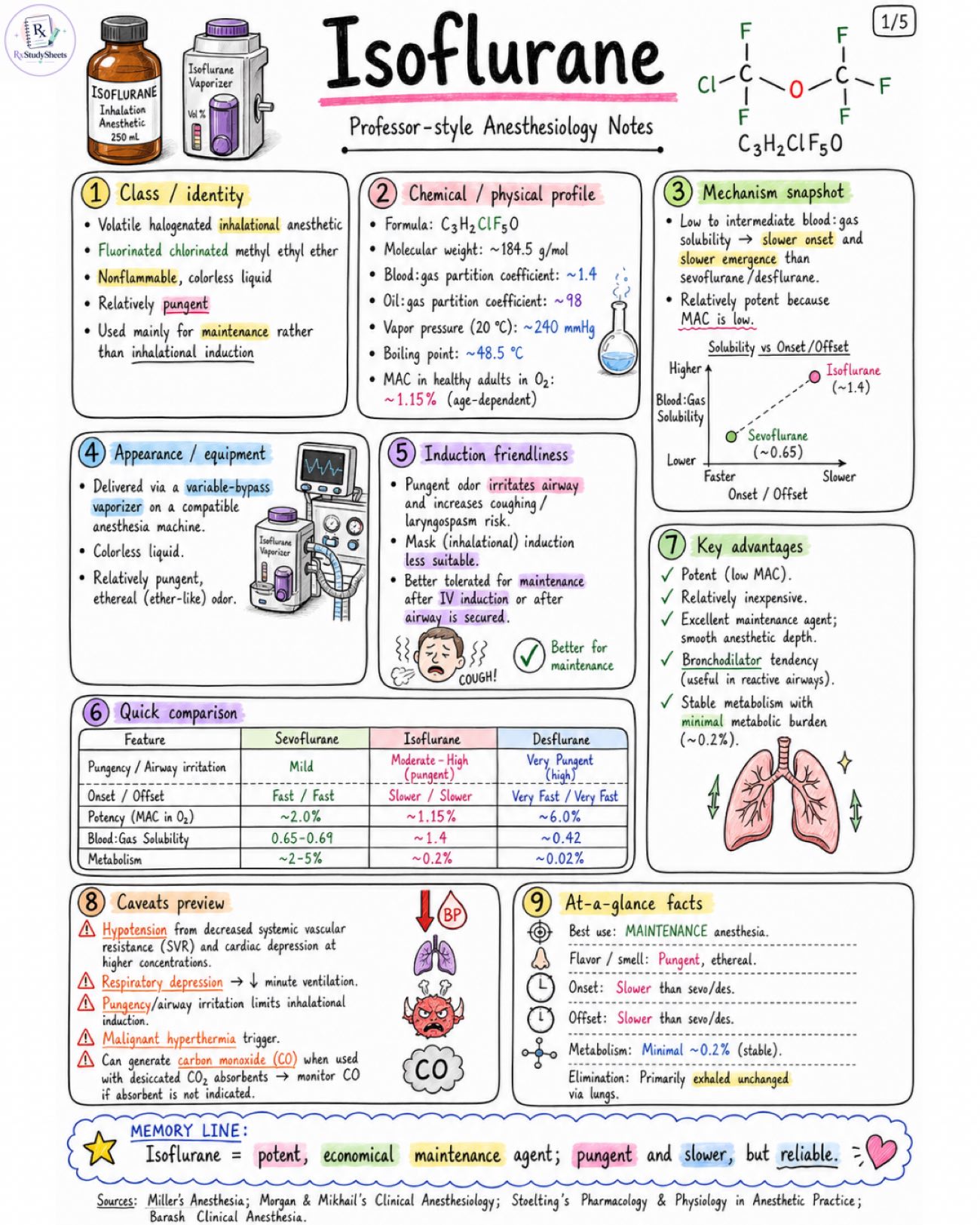
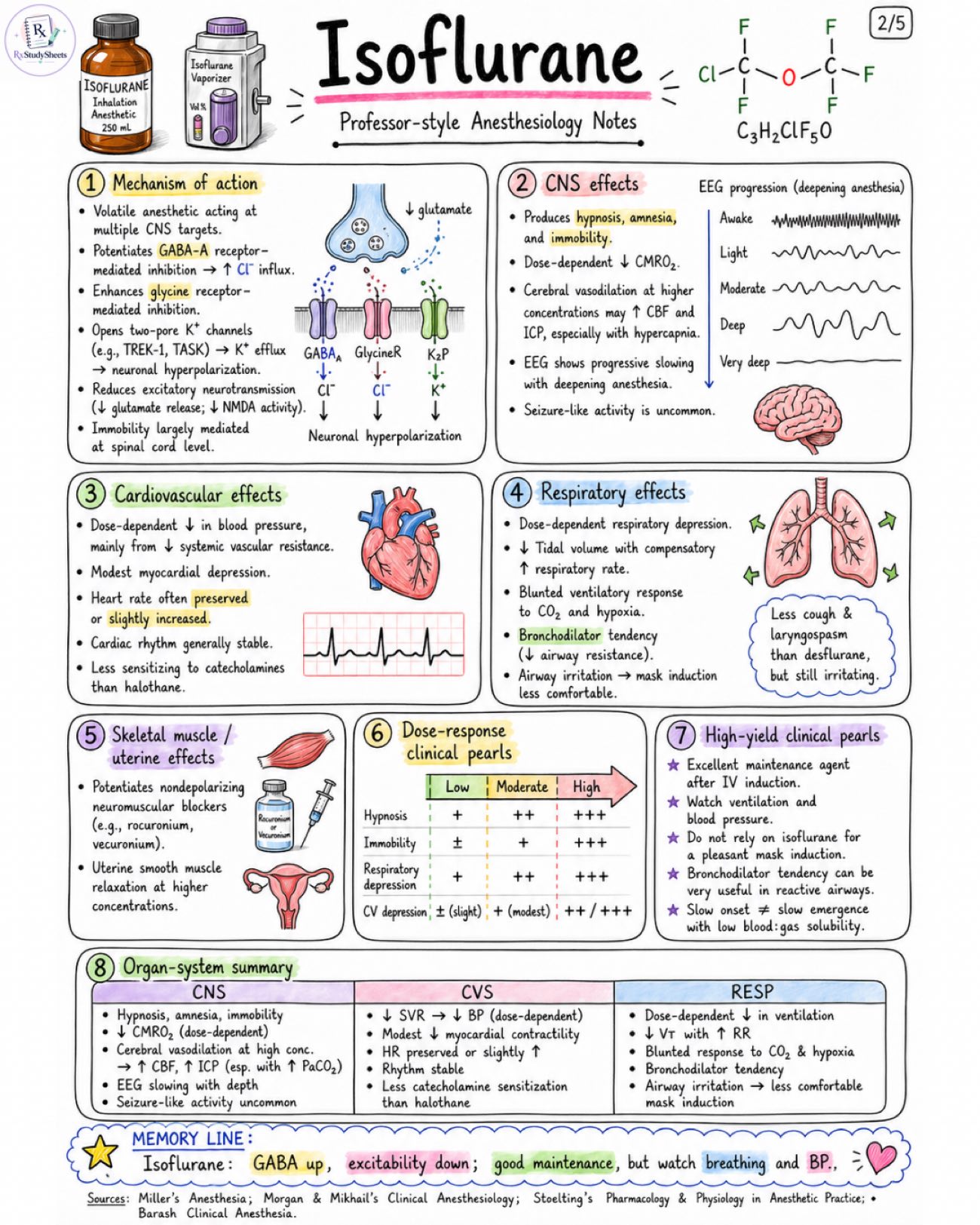
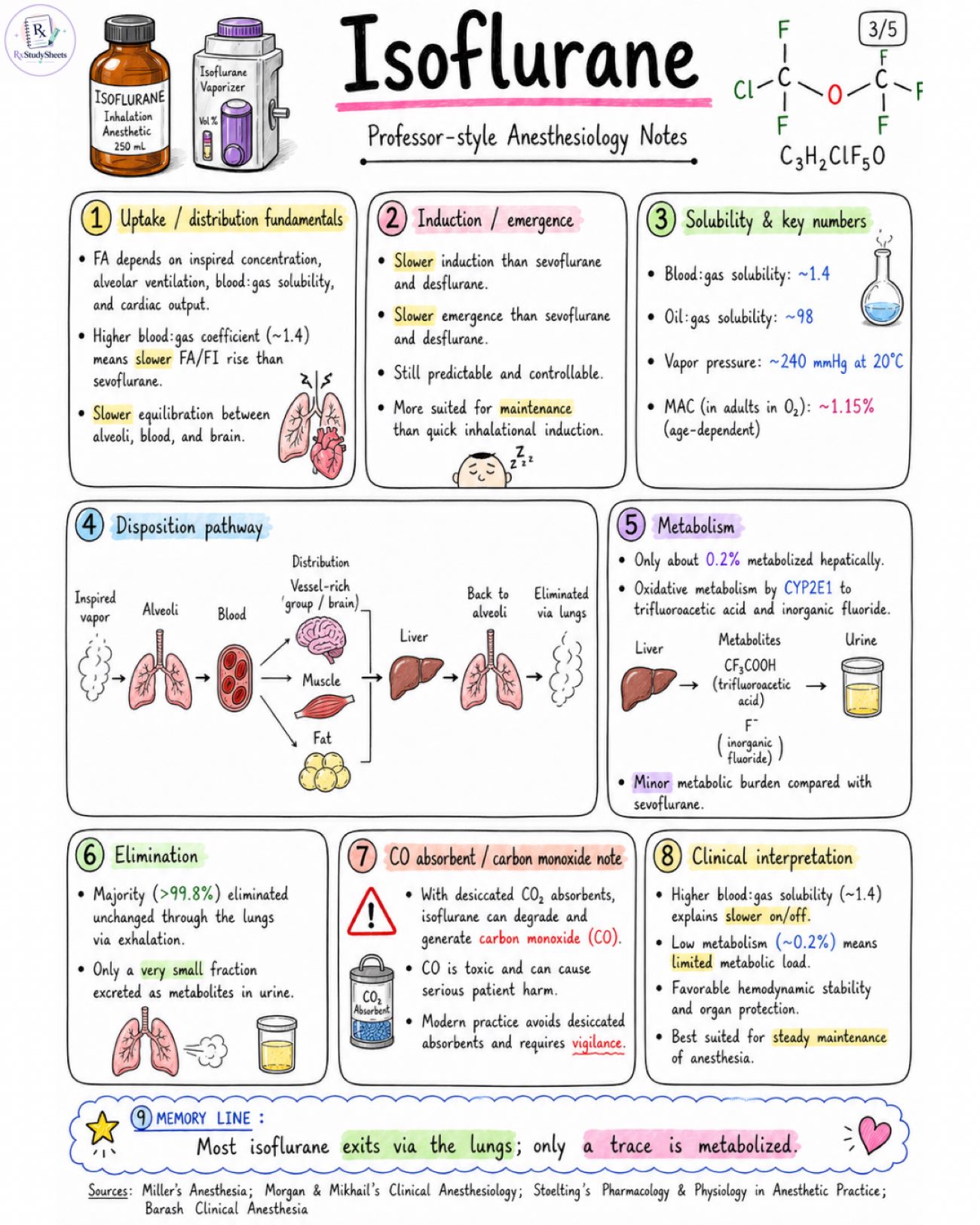
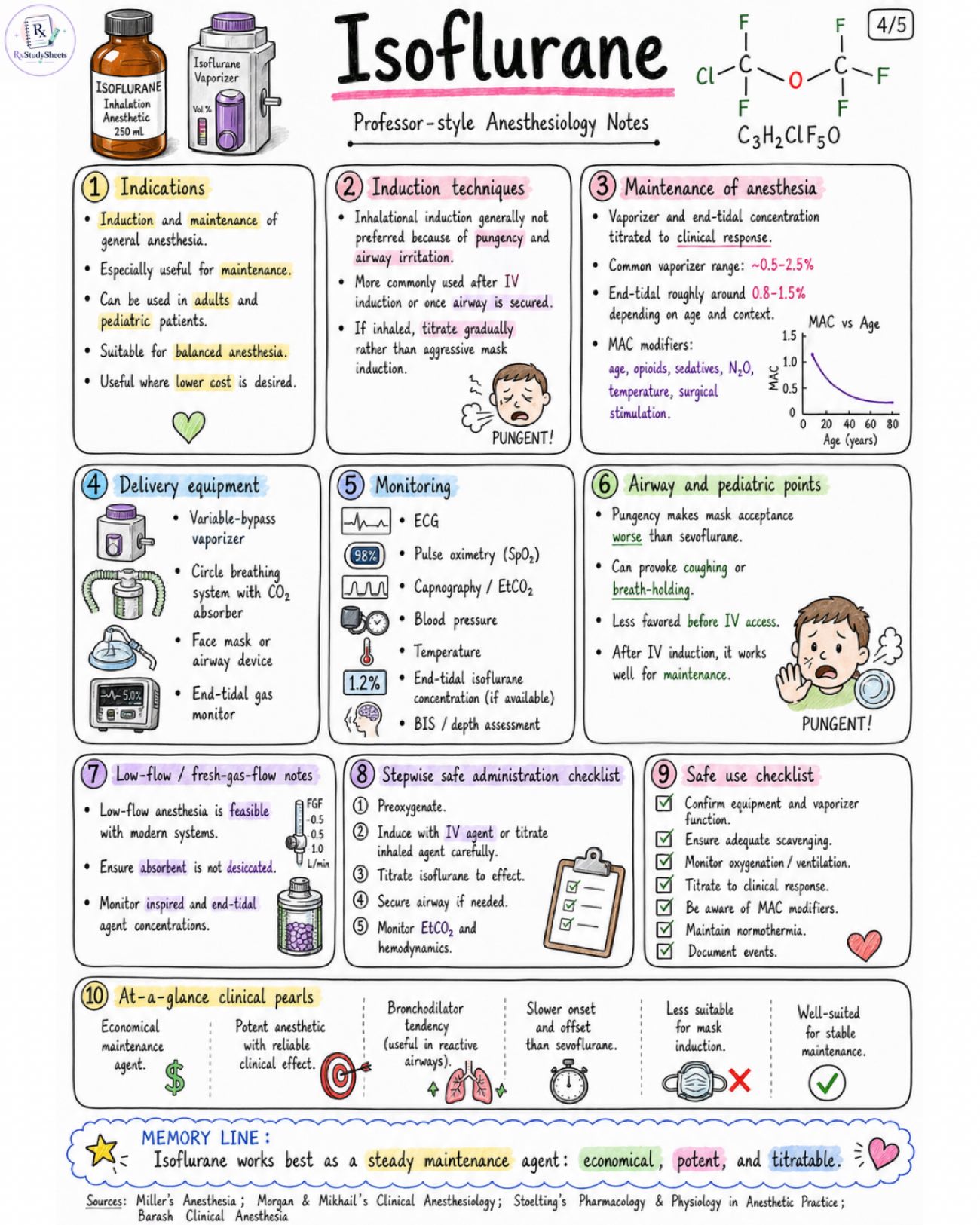
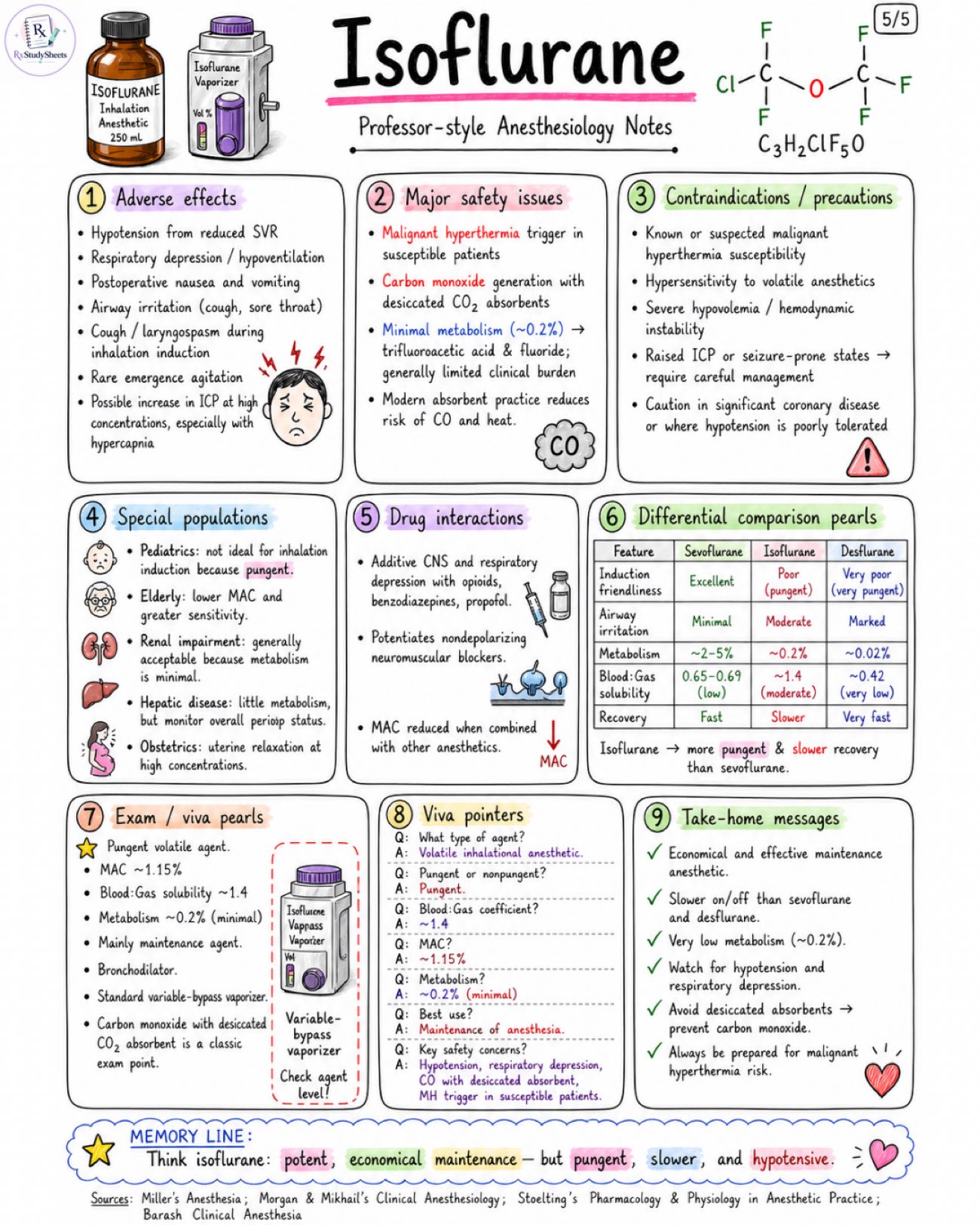
Isoflurane notes about properties, pharmacology, adverse effect, MAC value, with all standard book references. Class / identity: - Volatile halogenated inhalational anesthetic - Fluorinated chlorinated methyl ethyl ether - Nonflammable, colorless liquid - Relatively pungent - Used mainly for maintenance rather than inhalational induction Chemical / physical profile: - Formula: C3H2ClF5O - Molecular weight: ~184.5 g/mol - Blood:gas partition coefficient: ~1.4 - Oil:gas partition coefficient: ~98 - Vapor pressure (20 °C): ~240 mmHg - Boiling point: ~48.5 °C - MAC in healthy adults in O2: ~1.15% (age-dependent) Mechanism snapshot: - Low to intermediate blood:gas solubility → slower onset and slower emergence than sevoflurane/desflurane - Relatively potent because MAC is low Appearance / equipment: - Delivered via a variable-bypass vaporizer on a compatible anesthesia machine - Colorless liquid - Relatively pungent, ethereal (ether-like) odor Induction friendliness: - Pungent odor irritates airway and increases coughing/laryngospasm risk - Mask (inhalational) induction less suitable - Better tolerated for maintenance after IV induction or after airway is secured Quick comparison: - Feature: Sevoflurane, Isoflurane, Desflurane - Pungency / Airway irritation: Mild, Moderate - High (pungent), Very Pungent (high) - Onset / Offset: Fast / Fast, Slower / Slower, Very Fast / Very Fast - Potency (MAC in O2): ~2.0%, ~1.15%, ~6.0% - Blood:Gas Solubility: 0.65-0.69, ~1.4, ~0.42 - Metabolism: ~2-5%, ~0.2%, ~0.02% Caveats preview: - Hypotension from decreased systemic vascular resistance (SVR) and cardiac depression at higher concentrations - Respiratory depression → ↓ minute ventilation - Pungency/airway irritation limits inhalational induction - Malignant hyperthermia trigger - Can generate carbon monoxide (CO) when used with desiccated CO2 absorbents → monitor CO if absorbent is not indicated Key advantages: - Potent (low MAC) - Relatively inexpensive - Excellent maintenance agent; smooth anesthetic depth - Bronchodilator tendency (useful in reactive airways) - Stable metabolism with minimal metabolic burden (~0.2%) At-a-glance facts: - Best use: MAINTENANCE anesthesia - Flavor / smell: Pungent, ethereal - Onset: Slower than sevo/des - Offset: Slower than sevo/des - Metabolism: Minimal ~0.2% (stable) - Elimination: Primarily exhaled unchanged via lungs Image 2: Mechanism of action: - Volatile anesthetic acting at multiple CNS targets. - Potentiates GABA-A receptor-mediated inhibition → ↑ Cl- influx. - Enhances glycine receptor-mediated inhibition. - Opens two-pore K+ channels (e.g., TREK-1, TASK) → K+ efflux → neuronal hyperpolarization. - Reduces excitatory neurotransmission (↓ glutamate release; ↓ NMDA activity). - Immobility largely mediated at spinal cord level. CNS effects: - Produces hypnosis, amnesia, and immobility. - Dose-dependent ↓ CMRO2. - Cerebral vasodilation at higher concentrations may ↑ CBF and ICP, especially with hypercapnia. - EEG shows progressive slowing with deepening anesthesia. - Seizure-like activity is uncommon. Cardiovascular effects: - Dose-dependent ↓ in blood pressure, mainly from ↓ systemic vascular resistance. - Modest myocardial depression. - Heart rate often preserved or slightly increased. - Cardiac rhythm generally stable. - Less sensitizing to catecholamines than halothane. Respiratory effects: - Dose-dependent respiratory depression. - ↓ Tidal volume with compensatory ↑ respiratory rate. - Blunted ventilatory response to CO2 and hypoxia. - Bronchodilator tendency (↓ airway resistance). - Airway irritation → mask induction less comfortable. Skeletal muscle / uterine effects: - Potentiates nondepolarizing neuromuscular blockers (e.g., rocuronium, vecuronium). - Uterine smooth muscle relaxation at higher concentrations. Dose-response clinical pearls: - Low: Hypnosis + - Moderate: Hypnosis ++, Immobility +, Respiratory depression ++ - High: Hypnosis +++, Immobility +++, Respiratory depression +++ High-yield clinical pearls: - Excellent maintenance agent after IV induction. - Watch ventilation and blood pressure. - Do not rely on isoflurane for a pleasant mask induction. - Bronchodilator tendency can be very useful in reactive airways. - Slow onset ≠ slow emergence with low blood:gas solubility. Organ-system summary: CNS: - Hypnosis, amnesia, immobility - ↓ CMRO2 (dose-dependent) - Cerebral vasodilation at high conc. → CBF, ↑ ICP (esp. with ↑ PaCO2) - EEG slowing with depth - Seizure-like activity uncommon CVS: - ↓ SVR → ↓ BP (dose-dependent) - Modest ↓ myocardial contractility - HR preserved or slightly ↑ - Rhythm stable - Less catecholamine sensitization than halothane RESP: - Dose-dependent ↓ in ventilation - ↓ VT with ↑ RR - Blunted response to CO2 & hypoxia - Bronchodilator tendency - Airway irritation → less comfortable mask induction Image 3: Uptake / distribution fundamentals: - FA depends on inspired concentration, alveolar ventilation, blood:gas solubility, and cardiac output. - Higher blood:gas coefficient (~1.4) means slower FA/FI rise than sevoflurane. - Slower equilibration between alveoli, blood, and brain. Induction / emergence: - Slower induction than sevoflurane and desflurane. - Slower emergence than sevoflurane and desflurane. - Still predictable and controllable. - More suited for maintenance than quick inhalational induction. Solubility & key numbers: - Blood:gas solubility: ~1.4 - Oil:gas solubility: ~98 - Vapor pressure: ~240 mmHg at 20°C - MAC (in adults in O2): ~1.15% (age-dependent) Disposition pathway: - Inspired vapor → Alveoli → Blood → Vessel-rich group / brain → Muscle → Fat → Back to alveoli → Eliminated via lungs Metabolism: - Only about 0.2% metabolized hepatically. - Oxidative metabolism by CYP2E1 to trifluoroacetic acid and inorganic fluoride. Elimination: - Majority (>99.8%) eliminated unchanged through the lungs via exhalation. - Only a very small fraction excreted as metabolites in urine. CO absorbent / carbon monoxide note: - With desiccated CO2 absorbents, isoflurane can degrade and generate carbon monoxide (CO). - CO is toxic and can cause serious patient harm. - Modern practice avoids desiccated absorbents and requires vigilance. Clinical interpretation: - Higher blood:gas solubility (~1.4) explains slower on/off. - Low metabolism (~0.2%) means limited metabolic load. - Favorable hemodynamic stability and organ protection. - Best suited for steady maintenance of anesthesia. Image 4: Indications: - Induction and maintenance of general anesthesia. - Especially useful for maintenance. - Can be used in adults and pediatric patients. - Suitable for balanced anesthesia. - Useful where lower cost is desired. Induction techniques: - Inhalational induction generally not preferred because of pungency and airway irritation. - More commonly used after IV induction or once airway is secured. - If inhaled, titrate gradually rather than aggressive mask induction. Maintenance of anesthesia: - Vaporizer and end-tidal concentration titrated to clinical response. - Common vaporizer range: ~0.5–2.5% - End-tidal roughly around 0.8–1.5% depending on age and context. - MAC modifiers: age, opioids, sedatives, N2O, temperature, surgical stimulation. Delivery equipment: - Variable-bypass vaporizer - Circle breathing system with CO2 absorber - Face mask or airway device - End-tidal gas monitor Monitoring: - ECG - Pulse oximetry (SpO2) - Capnography / EtCO2 - Blood pressure - Temperature - End-tidal isoflurane concentration (if available) - BIS / depth assessment Airway and pediatric points: - Pungency makes mask acceptance worse than sevoflurane. - Can provoke coughing or breath-holding. - Less favored before IV access. - After IV induction, it works well for maintenance. Low-flow / fresh-gas-flow notes: - Low-flow anesthesia is feasible with modern systems. - Ensure absorbent is not desiccated. - Monitor inspired and end-tidal agent concentrations. Stepwise safe administration checklist: 1. Preoxygenate. 2. Induce with IV agent or titrate inhaled agent carefully. 3. Titrate isoflurane to effect. 4. Secure airway if needed. 5. Monitor EtCO2 and hemodynamics. Safe use checklist: - Confirm equipment and vaporizer function. - Ensure adequate scavenging. - Monitor oxygenation / ventilation. - Titrate to clinical response. - Be aware of MAC modifiers. - Maintain normothermia. - Document events. At-a-glance clinical pearls: - Economical maintenance agent. - Potent anesthetic with reliable clinical effect. - Bronchodilator tendency (useful in reactive airways). - Slower onset and offset than sevoflurane. - Less suitable for mask induction. - Well-suited for stable maintenance. Image 5: Adverse effects: - Hypotension from reduced SVR - Respiratory depression / hypoventilation - Postoperative nausea and vomiting - Airway irritation (cough, sore throat) - Cough / laryngospasm during inhalation induction - Rare emergence agitation - Possible increase in ICP at high concentrations, especially with hypercapnia Major safety issues: - Malignant hyperthermia trigger in susceptible patients - Carbon monoxide generation with desiccated CO2 absorbents - Minimal metabolism (~0.2%) → trifluoroacetic acid & fluoride; generally limited clinical burden - Modern absorbent practice reduces risk of CO and heat Contraindications / precautions: - Known or suspected malignant hyperthermia susceptibility - Hypersensitivity to volatile anesthetics - Severe hypovolemia / hemodynamic instability - Raised ICP or seizure-prone states → require careful management - Caution in significant coronary disease or where hypotension is poorly tolerated Special populations: - Pediatrics: not ideal for inhalation indu